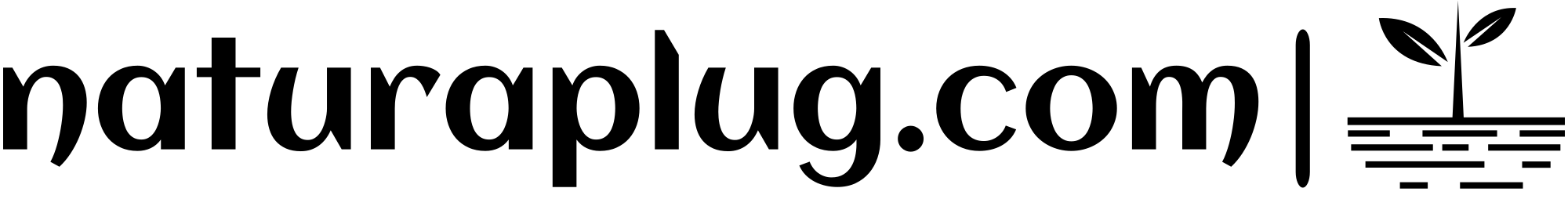Ultrasound is widely used to assess organs such as the ovaries, uterus, and thyroid in real time. Although it does not measure hormone levels directly, it can reveal structural patterns that reflect how hormones are influencing the body. In practice, these findings are interpreted alongside symptoms and lab tests to understand the full picture.
How Hormones Influence Imaging Findings
Hormones regulate tissue growth, fluid balance, and organ function, which is why changes in hormonal activity often show up as visible differences on ultrasound. Estrogen and progesterone drive cyclical changes in the uterine lining, while androgens influence ovarian structure. Thyroid hormones affect metabolism and can alter the size and internal texture of the gland.
Ultrasound captures the result of these processes over time. It reflects how tissues respond to hormonal signaling rather than measuring hormone levels themselves. Because of this, interpretation always depends on context, including the timing of the scan and the patient’s clinical presentation.
Timing Matters: Why the Menstrual Cycle Affects Results
One important but often overlooked factor is timing. In reproductive health, ultrasound findings can vary significantly depending on where a person is in their menstrual cycle.
For example, the endometrium naturally thickens and changes appearance as the cycle progresses. Similarly, ovarian follicles develop and regress in predictable patterns. If imaging is performed without considering cycle timing, normal physiological changes may be misinterpreted as abnormalities.
This is why clinicians often schedule ultrasounds at specific points in the cycle when evaluating hormonal concerns.
Common Ultrasound Findings Linked to Hormonal Conditions
In the ovaries, one of the most recognized patterns is the presence of multiple small follicles arranged around the periphery, often associated with polycystic ovary morphology. This appearance is commonly linked to androgen imbalance, although it is not diagnostic on its own and must be considered alongside symptoms and lab findings.
In the uterus, the endometrium reflects hormonal signaling throughout the cycle. A thin lining early in the cycle gradually thickens under estrogen influence before shedding. Disruptions in this pattern, such as persistent thickening or irregular structure, may suggest hormonal imbalance or ovulatory dysfunction.
The thyroid gland also demonstrates structural changes related to hormonal activity. Enlargement, nodules, or altered echogenicity can be observed on ultrasound. These findings may be associated with thyroid disorders, but they do not indicate function without laboratory confirmation.
Although the adrenal glands are not always clearly visualized on ultrasound, their hormonal output—particularly cortisol—can influence multiple systems. Chronic stress, for example, may indirectly contribute to patterns observed in reproductive or metabolic health over time.
What Ultrasound Can and Cannot Show
Ultrasound is highly effective at identifying structural differences, fluid-filled spaces, and tissue characteristics. However, it has limitations when it comes to functional assessment.
It cannot determine hormone levels, identify biochemical imbalances, or fully explain symptoms on its own. Two individuals with similar imaging findings may have very different hormonal profiles. This is why ultrasound is best understood as a complementary tool rather than a standalone diagnostic method.
When Imaging Alone Is Not Enough
A complete hormonal evaluation requires more than imaging. Clinicians typically combine several sources of information to reach a conclusion.
- Symptom assessment and medical history
- Laboratory testing of relevant hormones
- Imaging to identify structural patterns
This integrated approach reduces the risk of misinterpretation and allows for more accurate clinical decisions.
Connecting Symptoms, Hormones, and Imaging
Patients often seek evaluation after experiencing symptoms such as fatigue, irregular cycles, changes in weight, or fluctuations in mood. These symptoms may point toward hormonal involvement, but they are rarely specific on their own.
Ultrasound helps provide additional context by revealing how organs are responding. When combined with laboratory results and clinical evaluation, it becomes easier to distinguish between temporary fluctuations and more persistent hormonal conditions.
Supporting Hormonal Balance in Context
Hormonal health is influenced not only by medical conditions but also by everyday factors such as stress, sleep, and nutrition. These elements can affect how the body regulates key hormones and, over time, may influence the patterns observed in imaging.
Because of this, some individuals explore supportive approaches alongside medical care. Nutritional strategies and plant-based compounds have been studied for their role in supporting the body’s stress response and overall hormonal balance. Ingredients such as ashwagandha and maca root are often discussed in this context and are included in hormone balance product Hormify, which is designed to support energy levels, mood stability, and general hormonal wellbeing. These approaches are typically considered complementary and should be used alongside professional medical guidance rather than as a replacement.
A Holistic View of Hormonal Health
Hormonal balance is rarely determined by a single factor. Instead, it reflects the interaction between endocrine function, lifestyle, and overall health. Imaging adds an important layer by showing how these factors manifest structurally in the body.
By combining imaging, laboratory data, and clinical insight, clinicians can form a more complete understanding and guide appropriate next steps. For individuals, this reinforces the importance of viewing hormonal health as a long-term, multifaceted process rather than a single measurement or quick fix.
Key Takeaways
Ultrasound can reveal structural patterns that reflect hormonal activity, particularly in organs such as the ovaries, uterus, and thyroid.
However, it does not directly diagnose hormonal imbalance. Instead, it contributes to a broader evaluation that includes symptoms, laboratory testing, and clinical context.